Imagine you have just completed a 12-hour shift in the emergency room. You have taken blood samples, given IVs, and stitched up the wounds — all the time, you are running on coffee and adrenaline. Then, in a moment, a used needle slips.
You can’t breathe. You know what that means.
For millions of healthcare workers, this is not a scenario they think about. It is their existence.
So, What Is the Most Common Risk of Exposure to Bloodborne Pathogens for Healthcare Workers? The answer is needlestick and sharps injuries — and they occur much more frequently than people realize.
If you are an experienced RN, a med student on your first placement, or a hospital manager setting up safety measures, knowing this risk is more than good — it might be the difference between life and death. Probably yours.
Here you will find the main points about the bloodborne pathogens, the reason why needle stick injuries are the first on the list of exposure risks, who is most at risk, and what both workers and employers can do to be safe.
What Are Bloodborne Pathogens?
Let me first explain the exposure mechanism, while we know what kind of particle we are talking about.
Bloodborne pathogens are harmful microorganisms present in human blood and some other body fluids. If they manage to get inside the body – through an opening in the skin, a puncture wound, or contact with mucous membranes – they can result in severe, even fatal diseases.
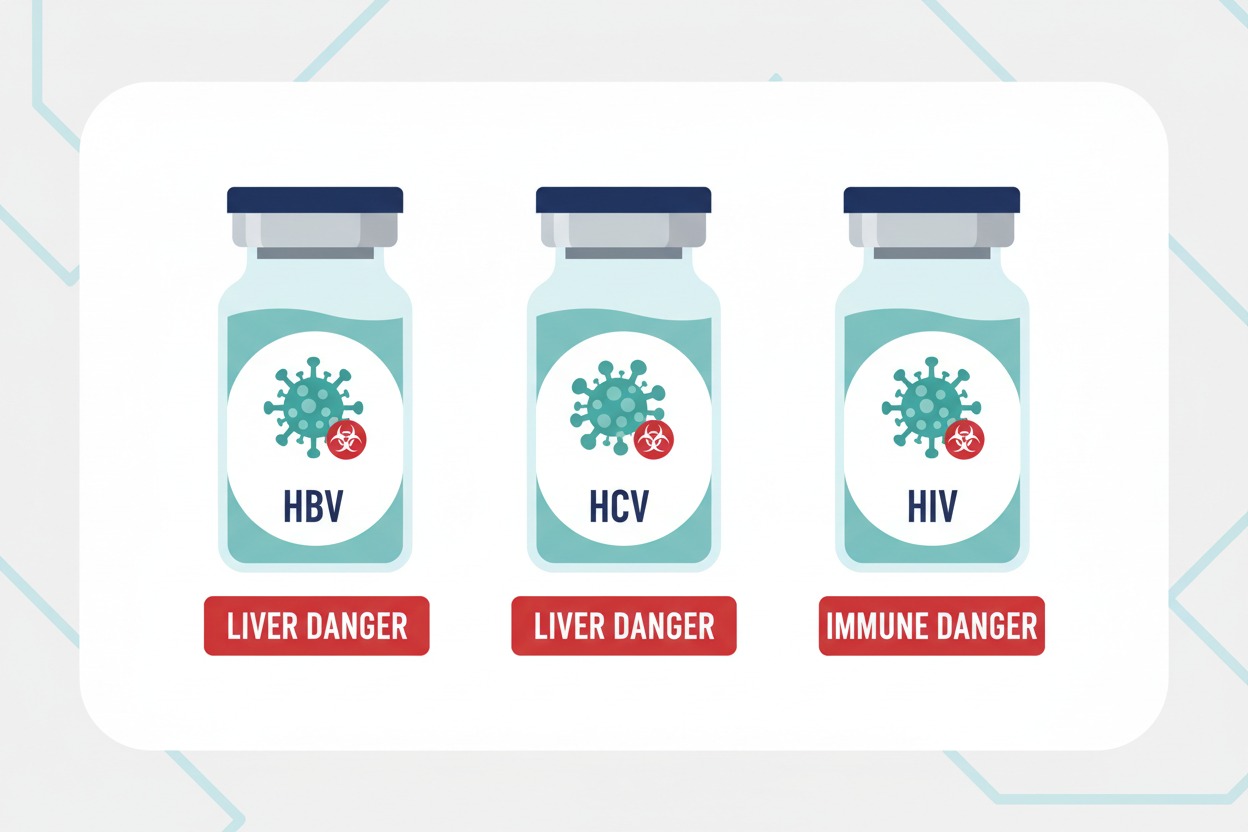
According to the CDC, the three most dangerous bloodborne pathogens for healthcare workers are:
- Hepatitis B Virus (HBV) — A highly infectious liver disease. Unvaccinated workers face the highest risk.
- Hepatitis C Virus (HCV) — Often called the “silent infection” because symptoms may not appear for years. It can lead to chronic liver damage, cirrhosis, and liver cancer.
- Human Immunodeficiency Virus (HIV) — The virus that causes AIDS. While less transmissible than HBV, any exposure is treated as a medical emergency.
The CDC also notes that bloodborne pathogens can transmit more than 20 other infectious agents, though HBV, HCV, and HIV remain the primary concerns in clinical settings.
What makes these pathogens very dangerous in healthcare is the exposure to blood and bodily fluids, which is constant and unavoidable. Almost no way exists in healthcare to perform the job without touching, drawing, or coming into contact with blood at some point, which is quite different from other workplaces.
What Is the Most Common Risk of Exposure to Bloodborne Pathogens for Healthcare Workers?
Injuries related to needlestick and sharps have been identified by research over several decades as a clear and consistent problem.
These refer to the harm caused by a needle, scalpel, lancet, suture needle, or any other sharp instrument being contaminated and accidentally piercing the flesh – this allows the transmission of bloodborne pathogens directly into the body.
According to the CDC, approximately 385,000 sharps-related injuries occur annually among hospital healthcare workers alone. More recent estimates from other sources place the number as high as 300,000 to 400,000 per year across all healthcare settings.
And here’s the part that should alarm every hospital administrator: at least 50% of needlestick injuries are never reported. The actual number of incidents is likely far higher than any official count reflects.
A systematic review and meta-analysis published in the journal BioMed Research International found that across a healthcare worker’s career, 56.2% experienced at least one needlestick injury, and the annual prevalence was 32.4%. That means roughly one in three healthcare workers gets injured by a sharp object in any given year.
This isn’t a rare accident. It’s an occupational epidemic hiding in plain sight.
When and How Do Needlestick Injuries Happen?
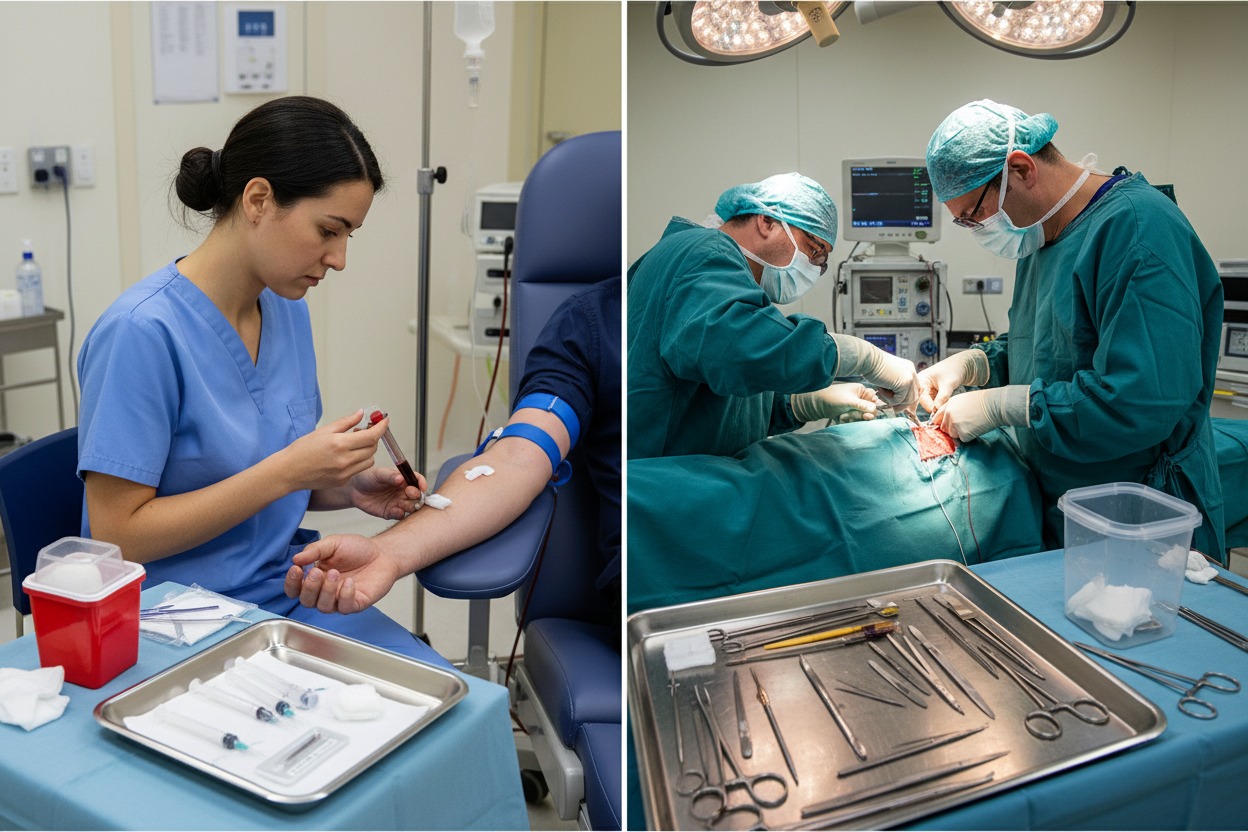
Needlestick injuries are not random events. Instead, they usually occur during certain tasks and conditions. The best way to preventing them is to know at which moments they are most likely happen.
Most Common Situations for Needlestick Injuries
Based on research and occupational health surveillance data, needlestick injuries most frequently occur during:
| Situation | Details |
|---|---|
| Needle recapping | Attempting to replace the cap on a used needle by hand — a practice now discouraged by OSHA |
| Blood draws and IV insertion | High-volume tasks performed quickly, often under pressure |
| Surgical procedures | Especially suturing, where curved needles and close hand-to-hand instrument passing increase risk |
| Disposal of sharps | Overfilled sharps containers, improper disposal techniques |
| Transfer of sharp instruments | Passing scalpels or needles between team members |
| Unexpected patient movement | A sudden jerk or startle during a procedure |
Research from a five-year surveillance study in Singapore found that intraoperative procedures accounted for 27.5% of all bloodborne pathogen exposure incidents, followed by minor procedures (15.6%) and splash incidents (12.7%). The highest-risk group? Physicians and surgeons, who reported 3.5 incidents per 1,000 healthcare workers per month.
A study from India reinforced this: needle pricks made up 86.2% of all reported exposures, with the Emergency Department and ICU being the most common locations.
Who Is Most Vulnerable?
Every healthcare worker is potentially at risk, but some roles face significantly higher exposure:
- Nurses — Due to high patient volumes and frequent IV and blood work
- Surgeons and surgical residents — Operating environments with dense sharps activity
- Phlebotomists — Blood draws as a primary job function
- Laboratory technicians — Handling samples and specimen tubes
- Housekeeping and janitorial staff — Often exposed to improperly discarded sharps in trash or linen
What Happens If a Needlestick Injury Occurs?

The moments after a needlestick injury matter enormously. The infection risk from a single exposure varies significantly by pathogen:
- Hepatitis B (HBV): For an unvaccinated worker, the risk of HBV infection from a single needlestick ranges from 6% to 30%, depending on the source patient’s viral load. This makes HBV by far the most transmissible bloodborne pathogen via needlestick.
- Hepatitis C (HCV): The average infection risk after a needlestick exposure to HCV-infected blood is approximately 1.8%.
- HIV: The average risk of HIV transmission from a needlestick is much lower — roughly 0.3% — but any risk is still unacceptable, and post-exposure treatment must begin quickly.
Immediate Steps After Exposure
If a needlestick or sharps injury occurs, here’s what should happen immediately:
- Wash the wound with soap and water for at least 15 seconds. Don’t squeeze or “milk” the wound.
- Flush mucous membranes (eyes, nose, mouth) with clean water or saline if splashed.
- Report the incident to a supervisor and the occupational health department without delay.
- Identify the source patient, if possible, for bloodborne pathogen testing.
- Begin post-exposure prophylaxis (PEP) if indicated — especially for HIV, where treatment must ideally begin within 2 hours.
Time is not on your side. The sooner post-exposure management begins, the better the outcome.
Other Routes of Bloodborne Pathogen Exposure

Needlestick injuries are the #1 risk, but they are not the only way bloodborne pathogens can be transmitted to the body. Other ways of exposure to healthcare workers include:
Mucous Membrane Splashes
Blood or bodily fluid splashing into the eyes, nose, or mouth represents a secondary but real exposure risk. Splash incidents accounted for 12.7% of bloodborne pathogen exposure events in one major multi-year surveillance study.
This is why face shields and goggles are part of standard PPE in any procedure involving blood.
Skin Contact (Non-Intact)
Skin that is intact and healthy acts as a fairly effective barrier against pathogens in the blood. However, if the skin is broken by cuts, rashes, dermatitis, or abrasions, the risk is considerably higher. For example, a healthcare worker with badly chapped hands, who comes into contact with blood without gloves will be exposed to an actual risk of infection.
Blood-to-Eye Contact
HCV infection from a blood splash to the eye has been reported, which is why eye protection is non-negotiable during procedures with splash risk.
How OSHA and Federal Law Protect Healthcare Workers

Decades ago, the federal government identified needle-stick injuries as an occupational hazard requiring serious attention. Therefore, safeguards have been legislated.
OSHA Bloodborne Pathogens Standard (29 CFR 1910.1030)
Established in 1991 and significantly updated in 2001, OSHA’s Bloodborne Pathogens Standard is the primary federal regulation protecting healthcare workers from exposure. It requires employers to:
- Develop and annually update a written Exposure Control Plan
- Implement engineering controls (like safety-engineered needles and sharps containers)
- Use work practice controls (single-handed needle recapping, no bending of contaminated sharps)
- Provide personal protective equipment (PPE) at no cost to the worker
- Offer Hepatitis B vaccination free of charge to all at-risk employees
- Conduct regular training and education on bloodborne pathogen risks
- Maintain records of all sharps injuries and incidents
The Needlestick Safety and Prevention Act (2000)
Congress went further in 2000 with the Needlestick Safety and Prevention Act, which required OSHA to update its BBP standard specifically to address sharps injuries. Among other things, this law required hospitals to use safer needle devices wherever feasible and to involve frontline healthcare workers in selecting and evaluating safety equipment.
The impact was real. Sharps-related injuries in non-surgical hospital settings decreased by 31.6% between 2001 and 2006 following the law’s passage — proof that policy changes save lives.
According to OSHA, compliance with the standard requires institutional commitment, interprofessional collaboration, and continuous education — not just a poster on the wall.
Expert Tips: Practical Ways to Reduce Your Risk

Understanding the risk is one thing. Reducing it is another. Here are evidence-based strategies that work:
For Individual Healthcare Workers
- Never recap needles by hand. Use the one-handed scoop technique or a mechanical recapping device.
- Always activate safety features on engineered needles and syringes immediately after use.
- Dispose of sharps immediately after use — don’t set them down or carry them across a room.
- Wear appropriate PPE for every procedure. Gloves are the minimum; add face shields when splash risk exists.
- Report every incident, no matter how minor. Unreported injuries prevent systemic change.
- Get vaccinated against Hepatitis B. It’s free under OSHA law, and it provides near-complete protection.
For Healthcare Employers and Administrators
- Adopt safety-engineered devices across departments. Studies show they significantly reduce injury rates.
- Involve frontline workers in selecting safety equipment — they know what actually works.
- Audit sharps container placement — containers should be at the point of use, not across the room.
- Foster a culture of safety where reporting injuries is encouraged, not stigmatized.
- Provide regular, meaningful training — not just annual click-through compliance modules.
The Psychological Toll of Bloodborne Pathogen Exposure
This is an issue hardly ever mentioned in occupational health literature, but it is significant.
If a healthcare worker suffers a needlestick injury from a source that might be infected, besides the physical risk, the worker may be overwhelmed emotionally as well. The period of waiting for follow-up blood donations – which can take several weeks – may be associated with anxiety, sleep problems, and fear.
Studies show that “occupational exposure to needlestick injury leading to infection might cause health problems that include anxiety ranging from mild to severe.” Psychologically, the trauma of work injury is acknowledged, and workers must be given support – a combination of clinical follow-up and emotional support resources, at a minimum.
Healthcare facilities should take the lead in providing counseling as a part of their post-exposure procedures.
FAQs: Bloodborne Pathogen Exposure in Healthcare
1. What is the most common risk of exposure to bloodborne pathogens for healthcare workers?
The major risk associated with needlestick and sharps injuries is their prevalence. Such injuries happen when a skin penetration through contaminated needles or sharp instruments is accidental, thereby providing a direct route for the pathogens, including HBV, HCV, and HIV, to enter the body. According to the CDC, hundreds of thousands of such injuries occur annually in healthcare environments.
2. Which bloodborne pathogen is most easily transmitted through a needlestick?
Hepatitis B (HBV) is definitely the most contagious among them. The chance of an unvaccinated individual getting the virus after a single stab with HBV-positive blood is estimated as 6%-30%. For relative comparison, the transmission rate of HCV is approximately 1.8%, and that of HIV is only 0.3% per needlestick incident.
3. Are healthcare workers required to be vaccinated against Hepatitis B?
As per OSHA, employers have a duty to provide the Hepatitis B vaccine series free of charge to employees who are exposed to blood or bodily fluids during the course of their work. Although workers have the right to refuse vaccination, they are obligated to sign a declination form. Being vaccinated is highly advisable — it offers a very high level of protection against the most easily spread bloodborne pathogen.
4. What should I do immediately after a needlestick injury?
Start by washing the wound with soap and water carefully, report the incident immediately to your supervisor and the occupational health team, try to locate the source patient for the test if it is possible, and if PEP is recommended, start post-exposure prophylaxis (PEP) without delay — particularly for HIV, where timing makes a significant difference.
5. Can bloodborne pathogens be transmitted through intact skin?
While intact and unbroken skin serves as a good barrier, they do not provide full protection. The major threat arises if blood or any infectious fluid comes in contact with non-intact skin, such as cuts, abrasions, eczema, or hands with cracks, or through mucous membranes like eyes, nose, and mouth. So even when you are not dealing with needles, gloves, face shields, and other PPE are still necessary.
Conclusion: Awareness Is the First Layer of Protection
Healthcare professionals dedicate themselves to helping others by healing. Paradoxically, the instruments that facilitate their noble work — needles, scalpels, and sutures — can also be their major source of danger at work.
Needlestick and sharps injuries are the top source of risk for healthcare workers’ exposure to bloodborne pathogens, accounting for the largest percentage of HBV, HCV, and HIV transmission events in healthcare environments. While the figures are distressing, the encouraging part is that injuries of this nature can be avoided.
With the right training, employing safety-disposed devices, regular PPE use, reporting as a rule, and a work environment that officially values staff safety, the hazard can be lessened significantly. Research indicates that progress is being made, but there is still much to be accomplished.
Keep in mind that if you are a healthcare worker, familiarize yourself with the procedures. Obtain vaccinations. Report all incidents. And never make peace with the notion that being stuck by a needle is merely “an aspect of the job.”
On the other hand, if you are an administrator or safety officer, your decisions regarding equipment, culture, and policy directly impact how many staff members under your supervision will be able to return home healthy after each work shift.
Start there. Protect the people who protect your patients.
Disclaimer: This article is intended for educational purposes only and does not constitute medical or legal advice. Always follow your institution’s specific safety protocols and consult occupational health professionals for guidance on bloodborne pathogen exposure.
Also Read: How Long Does It Take to Fill a Cavity? Everything You Need to Know


